Jump to paragraph
What Is The Pelvic Floor?
The pelvis, or the pelvic girdle, is a complex, funnel-shaped structure of bones located in the lowest portion of the abdominal cavity. It functions to support and connect the upper trunk with the lower trunk. The pelvis extends upwards into the abdominal cavity, and downwards into the perineum.
Since the pelvis has to support a considerable amount of body weight, it is strengthened by muscles, ligaments, and bony walls, protected from easily becoming injured or disabled. The pelvis consists of an anterior wall, a posterior wall, two lateral walls, and a pelvic floor.
The pelvis holds great significance in female anatomy, mainly because this part of the body is involved in the process of childbirth, so it is important to be aware of its structures and the vasculature that it contains. Healthy pelvic muscles and organs will ensure safe and easy delivery without any complications.
The pelvic floor is formed of muscles and fascias shaped in the form of a bowl and collectively referred to as the Pelvic Diaphragm. These muscles are the coccygeus, and the levator ani muscles and their fascias. The pelvic floor is highly susceptible to injury and prolapse.
Structure & Functions of The Pelvic Floor
The coccygeus muscle spans the lateral walls of the pelvic cavity, whereas the levator ani is attached to the pubic bone anteriorly, and the ischial spines posteriorly, along with thickening considerably in between these two bony points to strengthen the pelvic floor and reinforce it.
The levator ani has three parts (Puborectalis, Pubococcygeus, Iliococcygeus), which contribute to its strength. The levator ani muscle remains actively contracted the majority of the time, which thus enables it to:
- Maintain urinary and fecal continence
- Provide support and protection to the bladder, uterus, cervix, vagina, and the rectum
- Impart support to the abdominal cavity structures during periods of extreme stress
- Fix trunk posture when the upper limbs are exerting (lifting heavy weights, during strenuous exercise, etc.)
Pelvic Floor Dysfunction
The pelvic floor or the pelvic cavity, in general, is supported by several muscles which impart strength to it, enabling it to support different organs and perform a variety of jobs. However, under certain conditions, such as during childbirth, these muscles may be subjected to a lot of stress. Excess stress may lead them to be injured or torn and lose their active state of contraction, which further complicates things as it interferes with the individual’s normal functions. These conditions are fairly common in women, although they may affect men too.

Childbirth is the most common cause of pelvic floor dysfunction. | Source: freepik.com
In this condition, there is a loss of coordination between the pelvic floor muscles because they do not relax completely. This leads to poor and imbalanced nonsynchronous performance and may even cause the organs to prolapse.
Many conditions can cause the pelvic floor to dysfunction; some of them include:
- Childbirth
- Trauma
- Nerve damage
- Old age
- Post-surgery complication, or tearing
- Obesity
Whatever the cause may be, a wide range of symptoms is experienced by the patient, leading to the condition being finally diagnosed. Some common signs and symptoms experienced by the patient are:
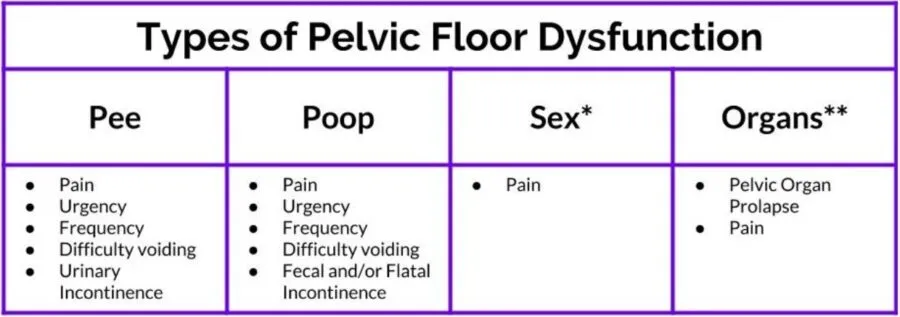

* There may be other problems related to sex (such as low libido) which are not a pelvic floor problem. ** There are many other conditions specific to the pelvic organs, gastrointestinal system, etc. Source: liftlaughkegel.com
Pelvic floor dysfunction can cause urinary incontinence. | Source: freepik.com
Treatment of Pelvic Dysfunction
As soon as a patient is diagnosed with pelvic floor dysfunction, the condition must be treated immediately to avoid further consequences. The condition in itself may be quite embarrassing, inconvenient, and painful for the patient, so it should be treated as early as possible.
There are many treatment options suggested for the patient, depending upon the damage and severity of the affected area. This condition has high cure rates, and it can be treated without the need for a surgical procedure, which is even better.
Here are a few common treatment plans used for pelvic floor dysfunction:
1. Pelvic Floor Physical Therapy
This is the most helpful and preferred among all treatment options. Even though it has been highly underestimated for years, this is the only reliable option that, although slow, brings fruitful results in the long-run. These exercises help patients with pelvic dysfunction in reducing the symptoms of incontinence of urine and feces, painful intercourse, and help to strengthen the muscles all together. It can be subdivided into a range of different exercises that can easily be done at home.
- Kegel’s: This is a pelvic muscle training method that focuses on strengthening the muscles by causing them to contract and relax simultaneously. It is extremely beneficial for patients with urinary incontinence issues.
- Glutes: This exercise greatly helps in activating the pelvic floor muscles, along with the glutes and the hamstrings.
- Squats: Squats help with improving muscle contraction by increasing the strength of the muscles.

Pelvic floor exercises can help reduce the symptoms of pelvic floor dysfunction. | Source: Pexels/Li Sun
If these exercises are done regularly for at least 15 minutes, then a noticeable alleviation of symptoms is sure to be noticed in the patient within one month. They are extremely beneficial for pregnant women, who, if they start doing these exercises during pregnancy, can strengthen their muscles enough to prevent tears during delivery, and incontinence afterward.
It is up to a person’s preference as to whether they wish to do these exercises by themselves, or go to a professional therapist for guidance. A physical therapist can offer detailed education and training for the patient on their specific condition and ensure that the patient complies with all the instructions.
2. Biofeedback
This is a modern-day technique. The doctor or therapist uses special sensors to monitor the pelvic muscles’ conditions, and using these sensors helps them regain their old functions. This is an easy and painless technique and allows the patient to gain back their normal muscle movements.
3. Medications
Occasional and supportive medicines can be taken to relieve the symptoms of pain and constipation.
Bonus video: Female pelvic floor muscle – 3D animation
FAQs
What makes pelvic floor dysfunction worse?
Common factors that weaken the pelvic floor include childbirth, obesity, and the associated straining of chronic constipation. Women who are obese or overweight are especially prone to pelvic floor disorders. Other factors that can increase the risk include repeated heavy lifting and genetics.
What are the symptoms of pelvic floor dysfunction?
The common symptoms of pelvic floor dysfunction include:
- Chronic pelvic pain that radiates to the groin, abdomen, and back
- Painful sexual intercourse
- Strong or frequent urge to urinate
- Burning during urination
- Urinary incontinence
- Vaginal burning
- Painful menstrual periods
- Difficulty with defecation and constipation
What are the functions of the pelvic floor muscles?
Pelvic floor muscles have two important functions:
- Provide physical support to the pelvic viscera
- Constrictor mechanism to the anal canal, vagina, and urethra
What triggers pelvic floor dysfunction?
What happens during a pelvic exam?
How long does it take to strengthen the pelvic muscles?
References:
-
Allen, R.E., Hosker, G.L., Smith, A.R., Warrell, D.W. Pelvic floor damage and childbirth: a neurophysiological study. BJOG: An International Journal of Obstetrics & Gynaecology. 1990 Sep;97(9):770-9.
-
Bump, R.C., Mattiasson, A., Bø, K., Brubaker, L.P., DeLancey, J.O., Klarskov, P., Shull, B.L., Smith, A.R. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. American journal of obstetrics and gynecology. 1996 Jul 1;175(1):10-7.
-
Dumoulin, C., Cacciari, L.P., Hay‐Smith E.J. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane database of systematic reviews. 2018(10).
-
Woodley, S.J., Lawrenson, P., Boyle, R., Cody, J.D., Mørkved, S., Kernohan, A., Hay-Smith, E.J. Pelvic floor muscle training for preventing and treating urinary and fecal incontinence in antenatal and postnatal women. Cochrane Database of Systematic Reviews. 2020(5).
-
Hagen, S., Glazener, C., McClurg, D., Macarthur, C., Elders, A., Herbison, P., Wilson, D., Toozs-Hobson, P., Hemming, C., Hay-Smith, J., Collins, M. Pelvic floor muscle training for secondary prevention of pelvic organ prolapse (PREVPROL): a multicentre randomized controlled trial. The lancet. 2017 Jan 28;389(10067):393-402.
-
Bonde, E.H., Wei, X.K., inventors; Medtronic Inc, assignee. Pelvic floor muscle training. United States patent US 10,201,702. 2019 Feb 12.
-
Narayanan, S.P., Bharucha, A.E. A practical guide to biofeedback therapy for pelvic floor disorders. Current gastroenterology reports. 2019 May 1;21(5):21.
-
Richmond, C.F., Martin, D.K., Yip, S.O., Dick, M.A., Erekson, E.A. Effect of supervised pelvic floor biofeedback and electrical stimulation in women with mixed and stress urinary incontinence. Female pelvic medicine & reconstructive surgery. 2016 Sep 1;22(5):324-7.