Glaucoma is a medical condition in which your optic nerve is damaged. The damage to your vision is most often caused by abnormally high pressure in your eye. This increase in pressure can cause irreversible damage to the optic nerve, responsible for sending visual signals to your brain. If the injury worsens over time, glaucoma may end up causing permanent vision loss or even total blindness within a few years. As it is not yet possible to reverse vision loss from glaucoma, early detection and treatment become crucial.
Jump to paragraph
Glaucoma Causes
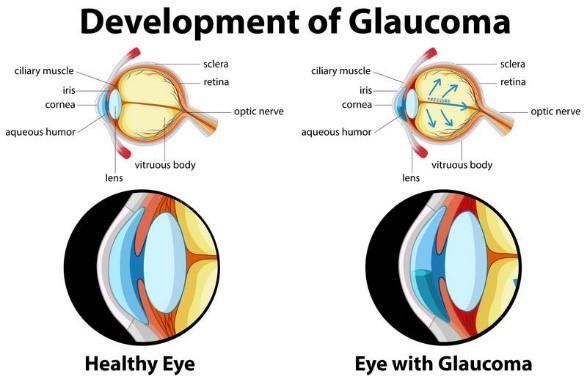
As stated above, glaucoma is a condition that manifests as a result of optic nerve injury caused by increased intraocular pressure. As the optic nerve gradually deteriorates, potential blind spots may begin to develop in your visual field, which ultimately worsens your vision. The elevated intraocular pressure is caused by the excess buildup of fluid that continuously flows in your eye, known as aqueous humor.
Usually, this fluid flows out of your eyeball through a mesh-like channel and drains out of your eye through a specialized tissue called the trabecular meshwork. This structure is present at the angle where the cornea and iris meet. Two phenomena can cause an increase in the intraocular pressure; either fluid itself is being overproduced, or the drainage system of the aqueous humor isn’t working efficiently. Consequently, the liquid cannot flow out of the eye at a standard rate and leads to an abnormal increase in eye pressure.
Glaucoma appears to have a hereditary component. In other words, a family history of glaucoma generally puts one at a higher risk of developing the disease. You usually don’t experience symptoms until later in life.
Another potential, but less common, causes of glaucoma include a chemical or direct blunt injury to your eye, blocked blood vessels in your eye, severe eye infection, and inflammatory conditions. Also, eye surgery to improve other medical conditions can aggravate glaucoma in your eye, but this is rare.
Risk Factors
Glaucoma is a condition that mostly affects people over 40, although children and even infants can have it. Below, we have listed some of the potential risk factors associated with a high incidence of developing glaucoma. You are more likely to be affected by glaucoma if you:
- Are over 40
- Have poor vision
- Have diabetes
- Have a family history of glaucoma
- Have had an eye injury
- Use cortisone (steroids)
- Have high eye pressure
- Are nearsighted (high degree of myopia)
- Have thinner corneas
- Black racial ancestry
- Suffer from heart disease, high blood pressure, or sickle cell anemia
Types of Glaucoma
Open-Angle Glaucoma
Open-angle glaucoma is the more popular form of the disease. The drainage angle between the iris and cornea remains open, but the trabecular meshwork becomes partially blocked. As a result, the eye pressure gradually increases, which ultimately puts a strain on the optic nerve. Once the pressure exceeds a specific safety limit, the optic nerve starts to deteriorate. This whole process happens very slowly, and you may end up losing your sight before becoming aware of the problem.
Close-Angle Glaucoma
Closed-angle glaucoma develops when the drainage angle formed by the iris and cornea gets blocked by the forward bulging of the iris. Consequently, the aqueous humor is unable to circulate through the eyeball freely, thus increasing the pressure. Some people may naturally have narrow drainage angles; this can significantly increase the risk of developing close-angle glaucoma. This type of glaucoma may occur suddenly. Acute close-angle glaucoma is considered a medical emergency.
Normal-Tension Glaucoma
In this version of glaucoma, the optic nerve is damaged even though your eyeball pressure is normal. The exact cause behind it is still unknown. A likely reason can be that your optic nerve is highly sensitive, or your optic nerve has a limited supply of blood. Having less blood flow to your optic nerve may cause atherosclerosis – a condition in which the arteries develop fatty deposits (plaque) that impair normal blood flow.
Low-Tension Glaucoma
In low-tension glaucoma, patients suffer from optic nerve damage and vision loss even when their intraocular optic pressure is within a healthy range. A potential risk factor for this type of glaucoma may be low blood pressure.
Congenital Glaucoma
The congenital type of glaucoma is present in infants born with defects in the drainage angle. As a result, the aqueous fluid is prevented from draining correctly and exiting from the eye normally. The usual manifestation of congenital glaucoma is the cloudy cornea, severe light sensitivity, and watery eyes.
Secondary Glaucoma
This variant of glaucoma develops due to complications due to certain medical conditions such as high blood pressure and diabetes. Other eye conditions like uveitis and cataracts also pose a significant risk for the development of secondary glaucoma. Moreover, the side effects of other medications or trauma to the eye may also play a role in the potential development of secondary glaucoma.
Pigmentary Glaucoma
In some cases, pigment granules from the iris detach and build up in the drainage channels. As a result, this buildup of pigment granules gradually blocks or slows down the fluid exiting the eye. That can significantly elevate the intraocular pressure and cause similar symptoms like glaucoma. Physical activities like running and jogging can aggravate this condition and facilitate the deposition of pigment granules in the drainage angle, resulting in intermittent intraocular pressure elevations.
Exfoliative Glaucoma
That is another type of glaucoma that can occur in either closed-angle or open-angle glaucoma. Deposits of brittle materials on the lens surface and in the drainage angle of the eye characterize exfoliative glaucoma. As a result of this accumulation, the drainage system becomes blocked, which slows down or completely prevents the flow of aqueous fluid from the eye. As a result, intraocular pressure is raised. This type of glaucoma is more prevalent in older adults and people of Scandinavian descent.
Symptoms
Many glaucoma patients have no apparent symptoms, especially in the early stages of the disease. Hence, regular visits to your eye doctor are crucial as they can diagnose and treat your glaucoma before you experience long-term vision loss. However, if a patient suffers from a severe or advanced form of glaucoma, like acute closed-angle glaucoma – it may manifest as:
- Severe throbbing eye pain
- Tunnel vision
- Eye redness
- Halos around lights
- Patchy vision
- Dilated pupils
- Blurred or foggy vision
- Headaches
- Nausea and vomiting
Glaucoma Tests & Diagnosis
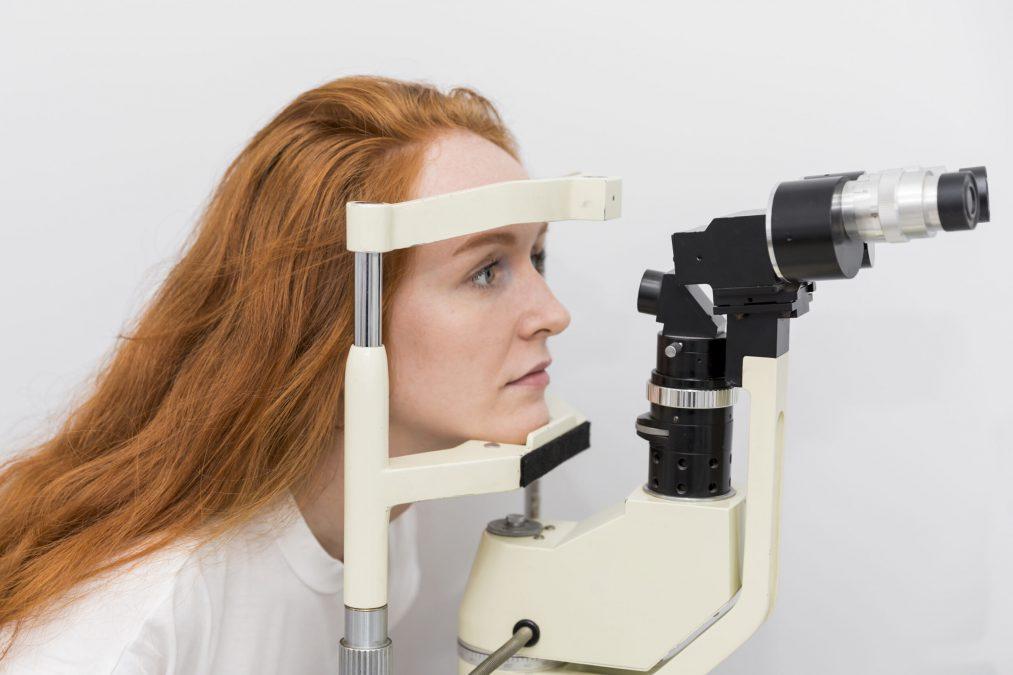
Glaucoma screening is a part of a standard, regular eye examinations. Ophthalmologists use intraocular pressure testing and evaluation of the optic nerves to diagnose glaucoma. A complete personal medical history and family history are also crucial for an accurate diagnosis of glaucoma. Your doctor may perform several tests, including:
- Visual Field Test – checks for areas of vision loss in your eye
- Gonioscopy – inspection of the drainage angle in the eye
- Tonometry – measures the intraocular pressure of the eyes
- Pachymetry – measures the corneal thickness
- Imaging Tests & Dilated Eye Examination – tests for the optic nerve damage

Ophthalmologist measuring the ocular tension in a female patient. | Photo credit: freepik.com
Treatment
Conservative treatment for glaucoma typically consists of eye pressure-reducing medications, usually in the form of eye drops. If a patient does not respond to this therapy, or if their glaucoma is particularly severe, surgery may be needed. The primary aim of surgery is to bring down the intraocular pressure inside the eye. There are numerous surgical treatment options available:
- Minimally Invasive Glaucoma Surgery (MIGS): This procedure reduces or eliminates the need for glaucoma medications. It requires only tiny surgical incisions and causes very little trauma to the eye compared to conventional glaucoma surgical methods. The goal is to increase the outflow of the aqueous humor from the eye to decrease the intraocular pressure and minimize damage to the optic nerve.
- Trabeculoplasty: A laser beam is used to clear the clogged drainage angle so that the fluid can quickly exit the eye without raising the intraocular pressure.
- Viscocanalostomy (Filtering Surgery): This procedure is opted for when all other treatment options fail, including laser surgery. Channels within the eyeball are opened up through surgery to improve the drainage of fluid.
- Aqueous Shunt Implant: This method is used for children or those with secondary glaucoma. To facilitate fluid drainage, a small silicone tube is inserted into the eye to prevent the intraocular pressure from raising to abnormal limits.

Eye drops for glaucoma can help in significantly reducing intraocular pressure. | Photo credits: freepik.com
Prevention
The following steps can help you detect glaucoma in the early stages; this is very important in preventing the disease or slowing its progress.
- Regular eye examinations: Comprehensive routine eye examination for detecting glaucoma in its early stages, even before it has caused significant damage to your optic nerve. The frequency of proper eye examination increases as age increases because of the increased risk of the disease.
- Know your family’s eye health history: Family history plays a significant role in this disease. Glaucoma tends to run in families. If a family member suffers from this disease, you are automatically at an increased risk of developing it. You will need to visit your eye doctor for frequent screening tests to ensure you’re safe.
- Exercise safely: Regular exercise is essential for everyone. However, if you are prone to developing glaucoma, moderate, and regular exercise can help prevent glaucoma by lowering the intraocular pressure.
- Take prescribed eye drops: The use of prescription eye drops is crucial for the treatment and management of glaucoma. The eye drops can significantly reduce eye pressure. To ensure maximum efficacy, strictly follow the medication plan your ophthalmologist prescribes for you.
- Wear eye protection: Another significant cause of glaucoma is external trauma. Be sure that your eyes are protected at all times. Wear eye protection equipment if you are in a situation where you can expect potential eye injury, i.e., using power tools, high-risk sports like in enclosed courts, etc.
Bonus video: What is glaucoma? | Causes, types, symptoms
FAQs
Is it possible for dogs to get glaucoma?
Yes, glaucoma is a typical dog’s disease. Please go to the veterinarian if you notice any of these glaucoma symptoms in dogs:
- Eye pain
- A watery discharge from the eye
- Lethargy, loss of appetite, or unresponsiveness
- Noticeable physical swelling and bulging of the eyeball
- Blindness
- Redness of the eye
- Cloudy cornea – cloudy or bluish cornea or exact part of the eye
- Squinting
- Tearing
- Avoidance of light
- Weak blink response
- Fluttering eyelid
Can glaucoma be stopped?
Yes, glaucoma can be cured. A summary of points from the article above:
- Minimally Invasive Glaucoma Surgery (MIGS)
- Trabeculoplasty
- Viscocanalostomy (Filtering Surgery)
- Aqueous Shunt Implant
How can I prevent glaucoma?
- Regular eye examinations.
- Know your family’s eye health history.
- Exercise safely.
- Take prescribed eye drops regularly.
- Wear eye protection.